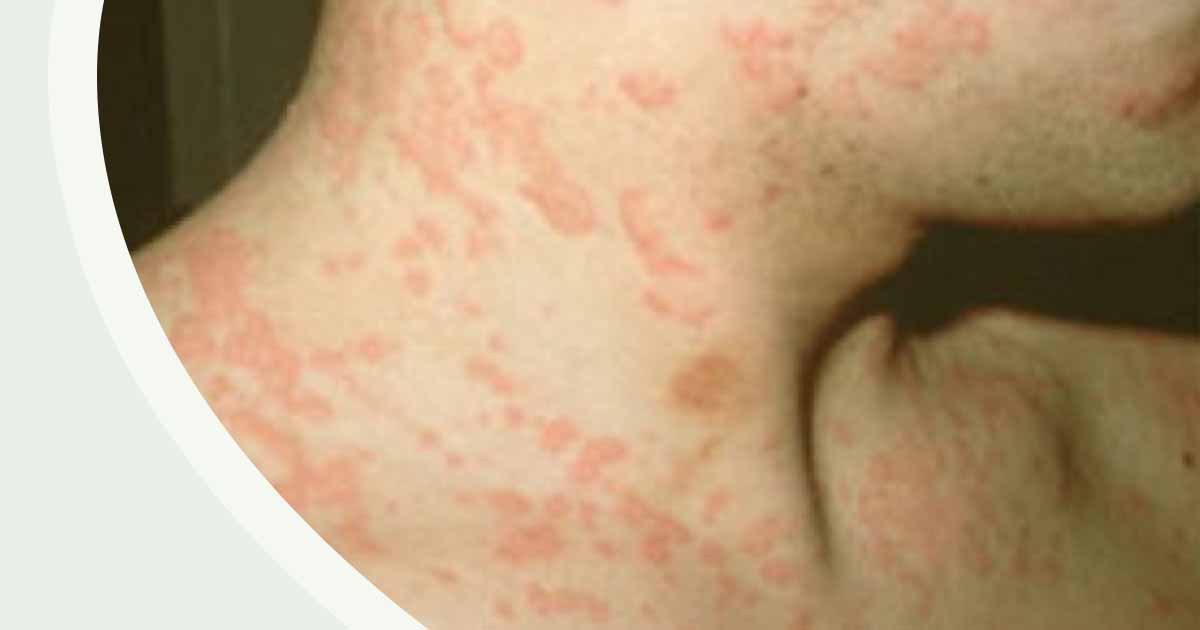
Aquagenic pruritus is a dermatological disorder that cause harsh pricking-like feeling/itch. The itching is triggered by the presence of water of any kind (including rainwater, seawater, bath/tap water, and even swimming pool water) on the skin. The water could be hot, cold, or tepid. Aquagenic pruritus is a variant of inducible pruritus.
Aquagenic pruritus can differ in harshness between a mild irritant to weakening and unbearable, resulting in a fear of taking a bath and water phobia. During the period of itching, the skin will appear normal.
The itching may appear immediately or hours after contact with water. The itching may last or go away after sometimes. It may develop at infancy, early childhood or adolescence.
Aquagenic pruritus is different from aquagenic urticaria, where the itch is accompanied by wheels. Among cutaneous feelings, the itching is of significance in dermatology and is still best described as it has been for centuries, as a displeasing sensation that provokes the longing to scratch.
When pruritus occurs during or after contact with water such as in bathing, it is called bathing pruritus, a form of aquagenic pruritus.
Various properties of water are known to be related to its ability to cause itching when used in bathing. These include the water temperature, physical characteristic/ionic content and the pH of the water, the soap used in bathing, sponging, and toweling afterward.
Areas of the body affected
The whole skin and palaver conjunctiva can itch, although there are great regional and individual differences in itch sensitivity. The perianal, perinatal areas, ear canals, arms, chest, abdominal wall, back, and nostrils are especially prone to itching. The peripheral receptors of itching are primarily confined to the superficially situated papillary dermis, which in most areas lies within the skin exterior.
The itching rarely affects the face, head, neck, soles, palms, mucosal surfaces.
In all possibilities, the very superficial nerve fiber endings and grid which function as receptors for itching are the same elements that function in the perception of superficial cutaneous pain.
What causes aquagenic pruritus?
The cause of aquagenic pruritus is not known. So, treatment of this condition is non-specific and insufficient in most patients, maybe because the pathogenetic and pathophysiological mechanisms leading to are not well understood.
Increased mast cell degranulation and subsequent release of histamine into circulation has been discussed. However, many patients with aquagenic pruritis do not respond well to anti-histamines, hence ruling out histamine as the only cause.
Cold causes degranulation of mast cells in both skin and the lungs. It may be a strong factor in the disease.
Some other factors have been discussed. They includd the release of acetylcholine, increase in skin fibrinolytic activity, release of neuropeptides like substance P, and inappropriate activity of sympathetic neurons system.
Severe aquagenic pruritus with intense itching may be associated with hematological disease, malignancy, and drugs. The best known associations being with:
- Essential thrombocytosis
- Myelodysplasia
- Lymphoblastic leukemia
- T-cell non-Hodgkin’s lymphoma
- Hypereosinophilic syndrome
- Hepatitis C
- Lactose intolerance (contribute to 25% of individuals with the condition)
- Systemic diseases like polycythemia vera, and urticaria (aquagenic pruritus is common in people with polycythemia vera)
- Medication such as bupropion, clomipramine.
- Antimalarial drug treatment like chloroquine
Blood disorders may manifest several years after the beginning of the itch, and an annual evaluation of hematology texture is suggested.
There are also genetic and hereditary disposition to the disease.
Diagnosis
There is no laboratory diagnosis. There is more of exclusion diagnosis, where possible disease like pruritus is ruled out.
Polycythermia vera is a differential diagnosis for aquagenic pruritus. However, all patients with the condition should be investigated for presence of polycythermia vera.
Complications of aquagenic pruritus
Aquagenic pruritus may cause complications such as:
- Severe itching, disturbing normal activities
- Lichen simplex chronicus
- Prurigo nodules and excoriations
- Insomnia leading to psychological disturbance.
- Phobia for water and bathing.
Who gets aquagenic pruritus?
- Mild water-induced itch is common
- More common in women, and in those who bathe in rainwater.
- It is generally much more severe in those with underlying associated hematological problems.
What are the clinical features of aquagenic pruritus?
Clinical characteristics include:
- Severe itching which can be burning, stinging, prick-like, on or after bathing or showering at any temperature is the cardinal symptom; this can develop within seconds of exposure or up to 15 minutes after contact with water has ceased.
- The sensation of the itch is symmetrical, and mostly affects the thighs and upper arms.
- During the period of itching, no visible skin changes occur or skin disease is found.
- You have ruled out all physical urticarias.
- Ultimately, the skin may show association and identification after repeated
- Pruritic reaction may occur after the itching
Treatment of aquagenic pruritus
Though there is no exact treatment for the condition, some therapeutic options are available. They are:
- Capsaicin cream
- Ultraviolet B phototherapy
- Oral antihistamines
- Psoralein Photochemotherapy
- Baking Soda Bath
- Sodium Bicarbonate emollients
- PUVA and Capasaicin
- PUVA and Astemizole
- Repeated PUVA
- Tight-fitting clotting
- Ultraviolet A/narrowband /UV B therapy
- Naltrexone
- Atenolol
- Propranolol
- Alcohol
READ ALSO: Different Types of Medical Swabs and the Uses
Home Treatment of aquagenic pruritus
There’s no cure for aquagenic hives. However, there are treatment options available to relieve symptoms.
- Always use warm water when bathing
- Stop using hard sponges on your skin
- Add some baking soda to your water
- Moisturize your skin immediately after having your bath
- You can add baby oil to your bathing water
If these don’t relieve symptoms, then you must see a doctor, in case of any underlying disease.
References:
- https://rarediseases.info.nih.gov/diseases/10278/aquagenic-pruritus/
- https://www.researchgate.net/publication/324721433_Aquagenic_Pruritus_A_Review_of_the_Pathophysiology-Beyond_Histamine
- https://dermnetnz.org/topics/aquagenic-pruritus
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3179019/