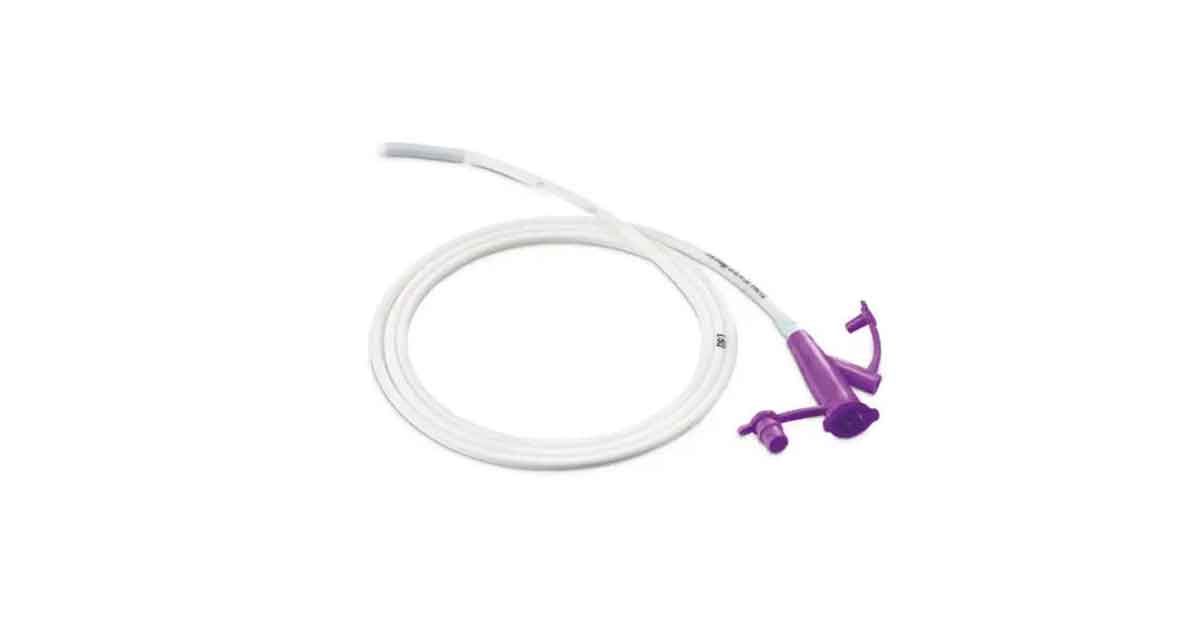
Orogastric tube is placed to decompress the stomach. It is used when there are high volumes of air or fluid in the stomach, limiting the compression of the chest compressions by inhibiting the return of venous blood to the thorax. High level of volume of air or fluid in the stomach also reduce the ability of the patient to be ventilated by bag-valve mask.
It is similar to the NG tube in both application and function except that it is placed through the mouth, unlike the NG tube that is placed through the nostril. However, both nasogastric tube and orogastric tubes are used to provide enteral nutrition.
OG tubes are preferred in patients receiving mechanical ventilation to reduce the risk of nasal bleeding and sinusitis. Orogastric tube placement is also better if there is coagulopathy or facial trauma.
The insertion of the orogastric tube involve the placement of the dual lumen tube into the stomach through the oropharynx to facilitate the gastric suctioning and decompression. The large lumen helps the suctioning of the gastric content and decompression, with the sump vent allowing the drawing in of air into the tube. This also prevents the suction eyelets from adhering and damaging the stomach.
It is a common procedure in clinical anesthesiology and intensive care to reduce gastric contents, and achieve gastric decompression.
Types and Sizes
The orogastric tube is made of suction eyelets, sump vent, length indicators, suction connector, and radio-opaque line (tube length).
- 18 Fr: Suitable for patients above 16 years
- 12 Fr: For patients below 16 years.
- 8 Fr: Neonates
Large tube placement (sed for Gastric Lavage)
- 8 Fr: Infants
- 10 to 16 Fr: Children
- 32 Fr (up to 50 F): Adult
Uses of Orogastric Tube
- Administration of medication
- Nutrition and feeding administration in patients with anatomical defects, critical illness.
- Gastric distension, which interferes with effective ventilation.
- Gastric suction and decompression in intubated patient.
- Cardiac arrest.
Contraindication
- A history of caustic ingestion or esophageal varices (risk of perforation)
- Basilar skull fracture
- Maxillofacial trauma
Insertion Procedure
The orogastric tube is passed into the oral cavity, through the oesophagus and into the stomach.
Equipment: Gastric tube (12 Fr or 16 Fr), water-soluble lubricating gel (lidocaine spray or jelly), stethoscope, laryngoscope, 30–60 mL catheter-tip syringe (not Luer lock), protective equipment like gloves and face shield, suction tube, tape.
- Measure the distance from the epigastrium to the corner of the mouth or nose, passing by the earlobe, to get the length of required tube.
- Lubricate the distal 7.5 to 10 cm of the tube using asceptic technique.
- Use the laryngoscope to visualize the esophagus.
- Insert the tube and move it to the desired depth.
- Check tube placement by auscultating over the epigastrium while injecting 20-30 mL of air down the tube using a 50 mL catheter syringe. Bubbling or “whooshing” sounds should be audible. If sounds are not heard, advance the tube by another 2.5-5 cm and re-check.
- Secure the tube with tape after it has been placed. Connect to suction at low vacuum.
- Connect the orogastric tube to a disposable drainage bag
References
- https://handbook.bcehs.ca/clinical-practice-guidelines/pr-clinical-procedure-guide/pr14-orogastric-tube-placement/
- https://www.ambulance.qld.gov.au/docs/clinical/cpp/CPP_Orogastric%20tube%20insertion.pdf
- https://www1.health.nsw.gov.au/pds/ActivePDSDocuments/GL2023_001.pdf
- https://fpnotebook.com/GI/Procedure/OrgstrcTb.htm