Antibiotics are antimicrobial substances or medicines used to stop bacterial infections, either by killing the bacteria or by inhibiting or slowing down the growth of the bacteria.
They are substances produced by a microorganism (wholly or partly by chemical synthesis).
We also known them as antibacterial agents, because they act specifically against bacteria.
We should note that antibiotics are not effective against viruses like influenza, HIV, common cold and so on.
Therefore, knowing the causative agent (microorganism) of a particular disease or infection is of utmost importance before commencing treatment.
Antiviral agents treat viral diseases.
Antifungal agents find their use in the cure and treatment of fungal diseases, and so on.
When bacteria invade the body system, the immune system (especially the white blood cells) naturally fights them.
But if the bacterial load is excess for the immune system to fight, antibiotics are being recommended and administered by a health practitioner.
The first antibiotic to be discovered is penicillin. A Scottish scientist, Alexander Fleming, discovered it in 1928.
Sources of Antibiotics
There are different sources of antibiotics used in clinical medicine today. They get some wholly from microorganisms; while they partly source some from microorganisms (they can either be synthetic or semi-synthetic).
However, the primary source of antibiotics is microorganism, used as mentioned irrespective of the method used as mentioned earlier.
Summarily, based on sources or origin, antibiotics can be grouped into:
- Natural antibiotics (sourced naturally and wholly from microorganisms)
- Synthetic antibiotics and
- Semi-synthetic antibiotics
The table below contains a list of different antibiotics and their different sources (microorganisms).
| ANTIBIOTICS | SOURCES (MICROORGANISMS) |
| Bacitracin | Bacillus licheniformis |
| Polymyxins | Bacillus polymyxa |
| Streptomycin | Streptomyces griseus |
| Tetracycline | Streptomyces aureofaciens |
| Penicillins | Penicillium species (Penicillium chrysogenum; Penicillium notatum) |
| Cephalosporins | Cephalosporium specothersies |
| Gentamycin | Micromonospora purpurea |
| Erythromycin | Streptomyces erythreus |
They produce synthetic antibiotics by making a prototype of natural drugs in the laboratory through chemical processes.
Examples of synthetic agents are sulphonamides, cotrimoxazole, quinolone, chloramphenicol, anti-tuberculosis and so on.
Semi-synthetic antibiotics are gotten from natural antibiotics by simply changing or alternating its chemical structure through the addition or removal of a specific chemical or functional group to increase its therapeutic effect.
Alternatively, semi-synthetic antibiotics are hybrids of natural and synthetic antibiotics.
The starting materials for semi-synthetic antibiotics are natural (microorganisms or plants), and involve the biological process of fermentation in the production.
Then, modification takes place finally in the laboratory by a chemical process or reaction.
Examples of semi-synthetic antibiotics include penicillins, ampicillin and amoxicillin (penicillin derivatives), cephalosporins, doxorubicin, and the anti-malarial drug, artemether.
Side Effects of Antibiotics
The side effects/adverse effects of antibiotics vary from individual to individual.
The major side effect of many antibiotics is gastrointestinal disruption such as vomiting, nausea, diarrhea, abdominal pain, loss of appetite, bloating and indigestion.
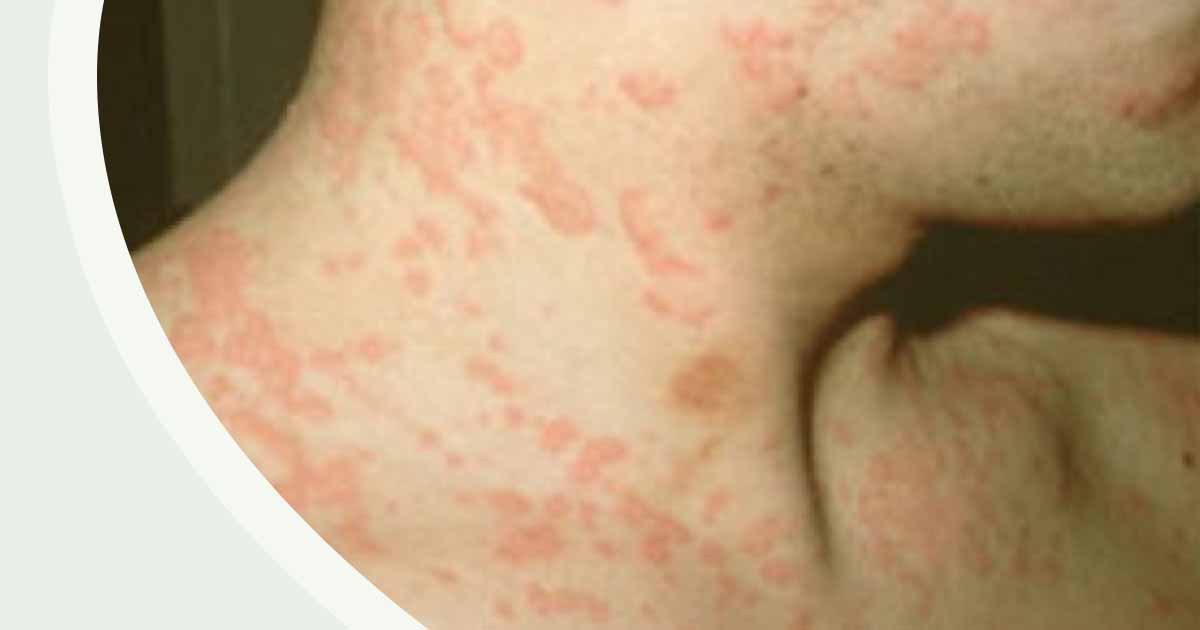
Allergic reactions can result from taking some antibiotics, such as penicillin and cephalosporins.
The reactions could range from mild-to-moderate cases of:
- Coughing
- A swollen, itchy skin rash (uticaria or hives)
- Wheezing
- Tightness of the throat, resulting in difficulties in breathing.
- In extreme and rare cases, a severe life-threatening reaction known as anaphylaxis can occur.
Classification of Antibiotics
Antibiotics have been classified based on several parameters, such as
- Source or origin of the antibiotics (Natural, synthetic and semi-synthetic antibiotics).
- Type of activity shown by the bacteria (bactericidal or bacteriostatic).
- Bacterial spectrum of activity (broad-spectrum or narrow-spectrum).
- Mechanism/mode of action (cell wall synthesis inhibitors, protein synthesis inhibitors, DNA inhibitors, RNA synthesis inhibitors, etc.)
- Route of administration (Oral, Intravenous or intramuscular) etc.
Source or origin of the antibiotics
We have explained this earlier in this post about the source of antibiotics. Read up for more details.
Type of activity
Antibiotics can either be bactericidal in action or bacteriostatic in action.
Bactericides or bactericides (Bcidal) stop bacterial infections by killing the bacteria.
They achieve this by interfering with the bacterial cell wall or cell content formation.
The bactericidal agents include β-lactam antibiotics, glycopeptide antibiotics, fluoroquinolones and aminoglycoside.
Bacteriostatics (Bstatic) inhibit the growth of bacteria by interfering general cellular metabolism of the bacteria like protein production, DNA replication, etc.
Bacteriostatic drugs include tigecycline, linezolid, macrolides, sulphonamides, tetracyclines and streptogramins.
Bacterial spectrum of activity
Antibiotics can be broad-spectrum or narrow-spectrum, depending on the range of its action against bacterial agents.
Broad-spectrum antibiotics act against a wide range of pathogenic bacteria.
Their actions are against the two major groups of bacteria, Gram-positive and Gram-negative bacteria.
They are used in empirical therapy where a bacterial infection is suspected but the group of bacteria is unknown or when infection with multiple groups of bacteria is suspected.
Ampicillin is a commonly used broad-spectrum antibiotic.
Other examples of broad-spectrum antibiotics are azithromycin, quinolones ec g. ciprofloxacin, doxycycline, minocycline aminoglycosides (except for streptomycin), amoxicillin/clavulanic acid (augmentin), carbapenems (e.g. imipenem), piperacillin/tazobactam, etc.
Narrow-spectrum antibiotics are effective against a selected and limited species or range of bacteria.
They either act on Gram-positive or Gram-negative bacteria, but not both.
Examples are: fidaxomicin, sarecycline, macrolides and vancomycin, etc.
N/B: Even though antibiotics are mostly used for treating infections, they can also be used prophylactically (prevention of infection), especially with surgery.
Mechanism/mode of action of antibiotics
A. Inhibitor of cell wall synthesis/ Peptidoglycan Inhibitors:
These antibiotics prevent the synthesis of peptidoglycan (a molecule that endues the cell strength on the bacteria for survival in the host) of bacteria. This exerts osmotic pressure on the cytoplasm; causing the swelling and lysing of the bacterial cell.
Examples are Beta-lactum; Penicillin, Bacitracin, Cycloserine, Phosphomycin, Cephalosporin, Vancomycin.
B. Inhibitor of protein synthesis:
These antibiotics bind to the ribosomes (the site of protein synthesis) of the bacteria. This causes blockage in the recognition of the protein codon. This finally leads to the prevention of amino acid chain growth.
Examples are streptomycin, aminoglycosides, fusidic acid, tetracycline, mupirocin, chloramphenicol, macrolides such as erythromycin.
C. Inhibitor of Nucleic acid synthesis:
These antibiotics bind and inhibit the synthesis of RNA polymerase. RNA polymerase sends gene instructions to the messenger RNA (mRNA). This interference stops the formation of new proteins.
Examples are quinolones, ciprofloxacin, nalidixic acid, metronidazole, nitrofurantoin, and so on.
D. Inhibitor of folic acid synthesis (Folate antagonistic):
Folic acid is essential for the synthesis of nucleic acids that make up bacterial DNA
Sulfonamide disrupts the folic acid pathway by targeting dihydropteroate synthase (DHPS). While trimethoprim inhibits dihydrofolic acid reductase (DHFR) and prevents the synthesis of folic acid by reducing dihydrofolic acid to tetrahydrofolic acid.
Examples are sulfonamide and trimethoprim.
E. Inhibitor of cytoplasmic membrane
These antibiotics cause membrane loss, which is because of rapid depolarization. This finally leads to the inhibition of the synthesis of protein, DNA and RNA.
Examples are polymyxin and colistin.
Classification of antibiotics based on the route of administration.
A. Oral or enteral antibiotics (Acid stable antibiotics)
They pass through the digestive tract or mouth.
Examples are Penicillin V, pivampicillin, pivmecillinam, doxycycline, rifampin and so on.
B. Parenteral route
Involves every other route other than the digestive tract or mouth. They take such antibiotics as injection or infusion. This route is used when the efficacy of the enteral or oral route is not predictable.
Parental route of antibiotic administration could be intravenous (in a vein) or intramuscular (in a muscle).
Examples of antibiotics that are administered intravenously are ampicillin or amoxicillin, azithromycin, etc.
Examples of intramuscularly administered antibiotics are Penicillin G benzathine, streptomycin, ceftriaxone (Rocephin) and so on.
In another post, we listed all the types of antibiotics with example.
Reference:
Ortho Bullets