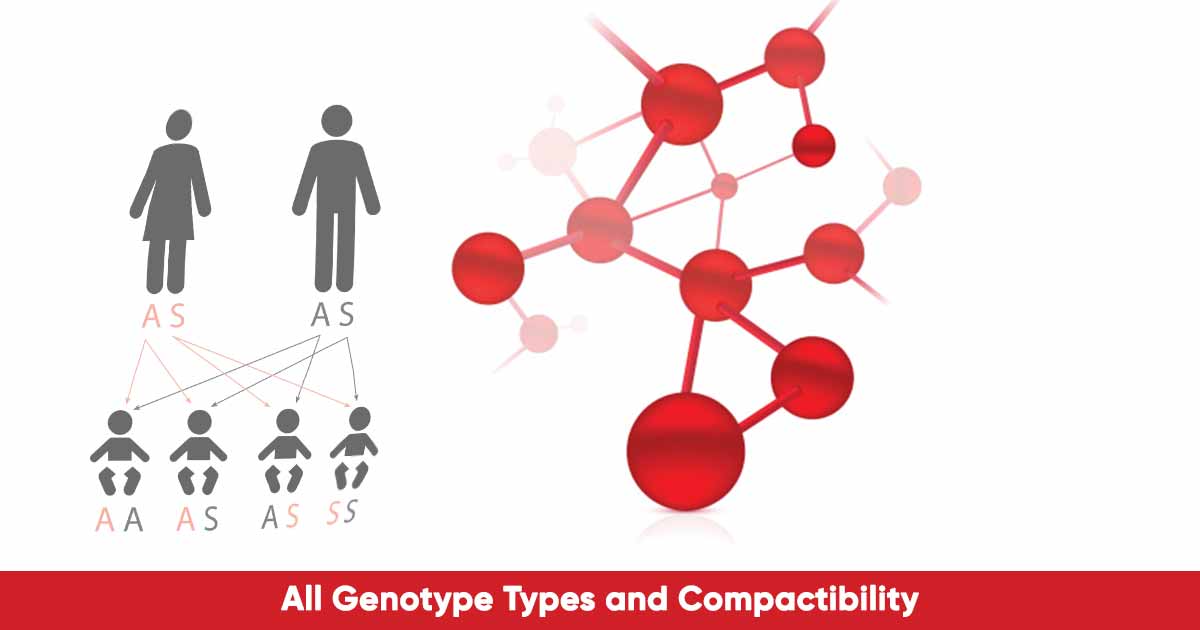
A carrier couple is a husband and wife with the sickle cell traits (Hemoglobin S) in their genotype, e.g., AS, and SS individuals. AS individuals, are advised not to marry each other, as there are possibilities of giving birth to a sickle cell patient. There are strongly advised to marry AA individuals, because AA has inherited two normal Hemoglobin A from both parents. This will cancel any possibility of producing a sickle cell patient.
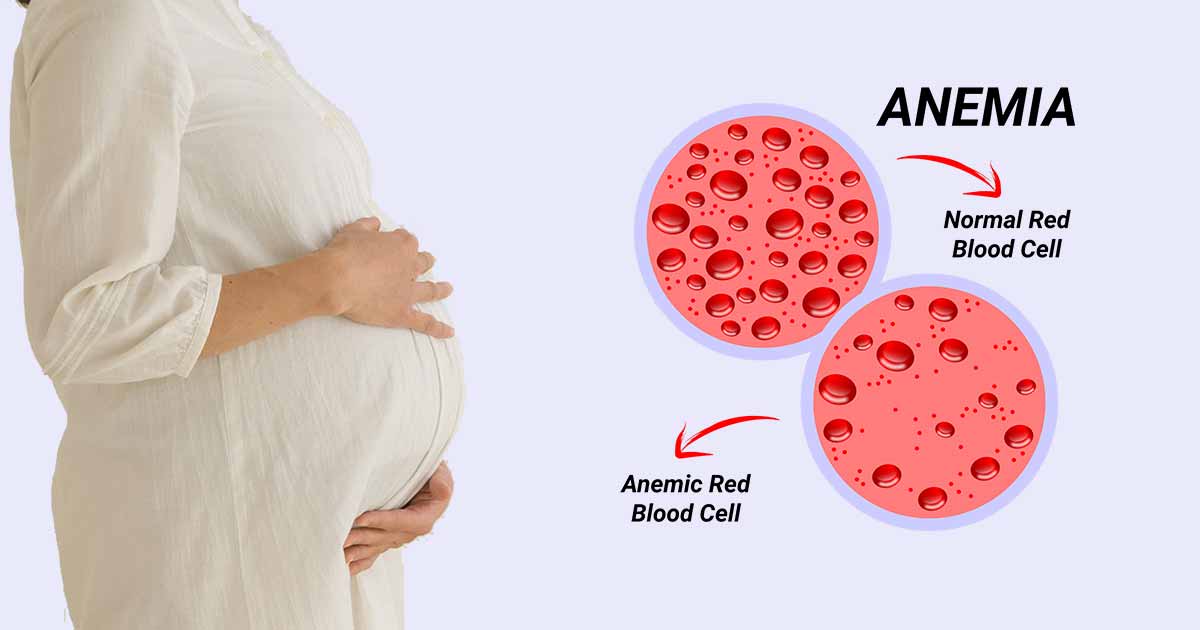
If a carrier couple marry, the possible outcome is that one out of four children will inherit two normal hemoglobin A (AA). Two out of four children will inherit one normal hemoglobin A and one sickle cell trait from both parents (AS). Also, one out of the four offspring can inherit one sickle cell trait from the mother and another sickle cell trait from the father, resulting in sickle cell anemia (SS).
However, if a carrier couple marry due to ignorance, or intentionally against medical advice and recommendation, there are method to prevent giving birth to children with sickle cell disease.
The first two methods are used in carrier couples with sickle cell traits to prevent the sickle cell disease in the baby before pregnancy. The method:
- In vitro fertilization, or IVF, with preimplantation genetic testing
In vitro fertilization:
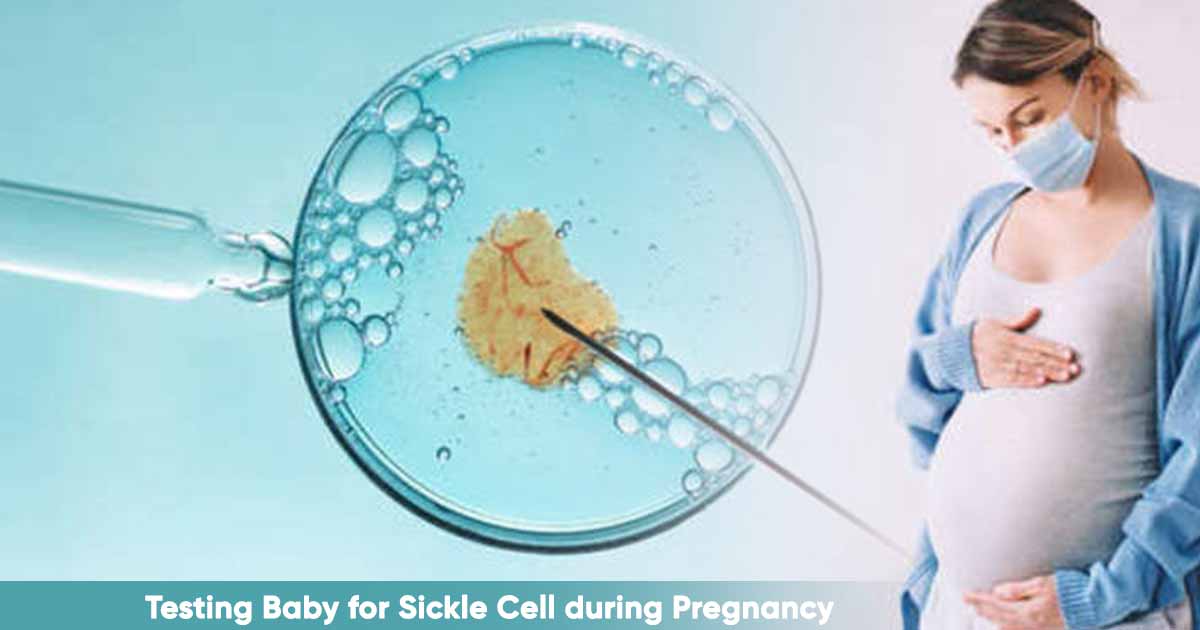
In vitro fertilization, medications are used to stimulate egg production in a woman. The eggs are extracted from the woman and fertilized with the donated sperm of the partner. The resulting embryo grows in the laboratory till the blastocyst stage, which is mostly 5 or 6 days. A sample of the embryo is taken, and analyzed using Preimplantation Genetic Diagnosis (PGD) or Preimplantation Genetic Testing for Monogenic Disorders (PGT-M).
Preimplantation Genetic Diagnosis (PGD) or Preimplantation Genetic Testing for Monogenic Disorders (PGT-M)
Preimplantation genetic testing (PGT) is a procedure that uses the day 5 embryos, that are generated from In Vitro Fertilization (IVF) process. It tests for chromosomal disorders such as sickle cell disease.
The lab takes samples from the couple and possibly other family members to test for the chromosome carrying the mutation in the family. The procedure involves the development of probes in the lab. Probes are small stretches of DNA that match familial mutation.
These probes can find other gene markers in the embryos, and check if the embryos are positive or negative for the condition. Additionally, the embryos can also be analyzed for other chromosomal issues (PGS or PGT-A).
Preimplantation genetic testing (PGT) reveals chromosomal issues, those affected with sickle cell, carrier cells and normal cells. The fertility specialist and the couple make a decision on which embryo to implant.
How to Test the Baby for Sickle Cell Disease
The other two methods are for couples who both have sickle cell traits, and the woman is already pregnant. The procedures are extreme, and the options include medical termination of the pregnancy if sickle cell is detected. They are:
- Amniocentesis, and
- Chorionic villus sampling (CVS)
Amniocentesis
In amniocentesis, a needle is placed through the womb of the woman, and a sample is collected from the amniotic fluid (the fluid where the baby floats in the womb). Since the amniotic fluid contains the cells from the baby, it can be tested in the laboratory to reveal the genetics of the baby.
Amniocentesis can determine an extra or missing chromosome, e.g., Down’s Syndrome (trisomy 21) where there are extra chromosome 21 in the body cells. Other genetic disorders it could detect include cystic fibrosis, sickle cell anemia or Tay Sachs Disease.
Amniotic fluid can also be tested to check if a baby will have spina bifida. A high level of a protein called alphafetoprotein (AFP) in the amniotic fluid is suggestive of spina bifida. Ultrasound test can confirm it.
An ultrasound scan is done before proceeding to ensure where the placenta and the baby are, and if they are twins.
This procedure is generally less painful, and is done between 16 and 18 weeks of the pregnancy. It has less and very minimal risk of miscarriage (1 in 100). Also, the procedure is an outpatient test.
This test result is available in three to four weeks. Medical termination of the pregnancy can be done in 19 to 20 weeks of pregnancy. It is important to note that most of the chromosomal abnormalities detected by amniocentesis are serious conditions, and medical termination may be a necessary option.
Amniocentesis is a reliable way to determine baby’s chromosomes, but the baby cell must grow in the lab. If this does not occur, further tests will be needed.
Chorionic Villus Sampling (CVS)
Unlike amniocentesis, this test is done around 9th or 10th week of pregnancy. Chorionic villus sampling (CVS) involves taking a small sample from the developing placenta by placing a thin tube through the cervix (neck of the womb).
Another method used in CVS, that is similar to the amniocentesis test, is by placing a needle in the womb, and using an ultrasound scanner to guide it.
Chorionic Villus Sampling (CVS) has an advantage over amniocentesis, as it can be done earlier (9th or 10th week of pregnancy). The result also comes out in one to two weeks after the procedure.
However, there are slightly more chances of miscarriage in CVS than amniocentesis. It is also a new method, and there could be little doubt on reliability.
References:
- https://www.thebridgeclinic.com/blog/how-to-prevent-your-baby-from-inheriting-sickle-cell-disease
- https://www.illumefertility.com/fertility-blog/how-ivf-and-genetic-testing-can-prevent-sickle-cell-anemia
- https://www.sicklecellsociety.org/resource/testing-baby-sickle-cell-pregnancy/#:~:text=It%20is%20possible%20to%20test,chorionic%20villus%20sampling%20(CVS).